Coughing and respiratory disease are quite common in cats. There are many causes but one is inflammatory airway disease which is sometimes called ‘asthma’.
The terms ‘feline asthma’ and ‘chronic bronchitis’ are often used interchangeably in cats and are used to describe chronic disease of the small airways (bronchioles) within the lungs. Other terms describing the same syndrome are ‘allergic airway disease’ and ‘allergic bronchitis’.
In human medicine, chronic bronchitis and asthma are two separate conditions (although some people have both). Asthma is usually an allergic condition where exposure to a trigger causes inflammation and narrowing of the airways. With chronic bronchitis, there is also inflammation of the airways and excessive mucous production. Environmental irritants may contribute to both conditions. The exact cause in most cases remains uncertain, and secondary bacterial infection is possible.
What are the signs of asthma or chronic bronchitis in cats?
The signs of asthma or chronic bronchitis vary in severity between individuals. In addition, the signs may be either persistent or episodic. Typical signs include:
- Persistent coughing (often in short bouts)*
- Laboured and/or fast breathing
- Noisy breathing and wheezing
- Difficulty in breathing (particularly seen in asthma)
*note that coughing in cats can look a little like the cat is trying to be sick, and may be mistaken for ‘hairballs’ as the cat may retch or gag after coughing with their neck stretched out. Taking a video to show your vet is the best way to establish if the cat is truly coughing.
Which cats develop asthma or chronic bronchitis?
Cats of any age, breed or sex can develop chronic airway disease. Most affected cats are adults, and typically 6-9 years of age, but signs can start in young cats or elderly cats as well. There is also a marked breed predisposition among Siamese and related breeds, strongly suggesting an inherited component to the disease in at least some cats.
How is asthma or chronic bronchitis diagnosed?
Cats with other diseases such as bacterial infections, pneumonia, foreign bodies, heart disease, airway parasites and lung cancer can present with similar clinical signs to asthma or chronic bronchitis so further investigations are usually needed to confirm a diagnosis. These may include:
- Blood tests
- Bronchoscopy – passing a small endoscope (camera) down into the lungs to look at the small airways
- Airway washes (bronchial or bronchoalveolar lavage) – this is a procedure performed under an anaesthetic that allows cells and fluid from the small airways to be collected and then examined for the presence of inflammatory cells, bacteria, cancer cells and other changes.
How is asthma or chronic bronchitis treated?
In practice, both are currently treated in the same way, although asthmatic cats may benefit more from bronchodilator therapy (to open the airways).
Generally, any secondary infections (with bacteria) should be identified and treated, and any predisposing or exacerbating causes identified and removed if possible. This would include:
- Managing any obesity (as this can worsen breathing difficulties)
- Identifying any potential irritants or allergens in the house, for example: pollens, use of perfumes or sprays, use of dusty cat litter, smoking in the house
- In some cats the disease may be seasonal or may occur only when the cat is in certain rooms. In these situations, it may be possible to track down an irritant or allergen that triggers the disease with careful investigations
In most cats, specific trigger factors cannot be identified (or cannot be avoided) and so symptomatic treatment will be required. This is mainly based around anti-inflammatory and bronchodilator therapy:
- Anti-inflammatory drugs– corticosteroids (glucocorticoids) such as prednisolone are potent anti-inflammatories that are used to achieve this. Treatment can be administered orally, with tablets or liquids, occasionally by injection, or by inhalation.
- Bronchodilator therapy– this is the use of drugs that relax the small muscles around the airways and help them to dilate. These are usually used along with corticosteroids (see above). They can also be given in the same three ways as anti-inflammatory drugs.
- Other drugs– some other drugs are used on occasions in cats – different types of anti-inflammatory drugs or drugs designed to block an allergic response
How are inhaled drugs administered to a cat?
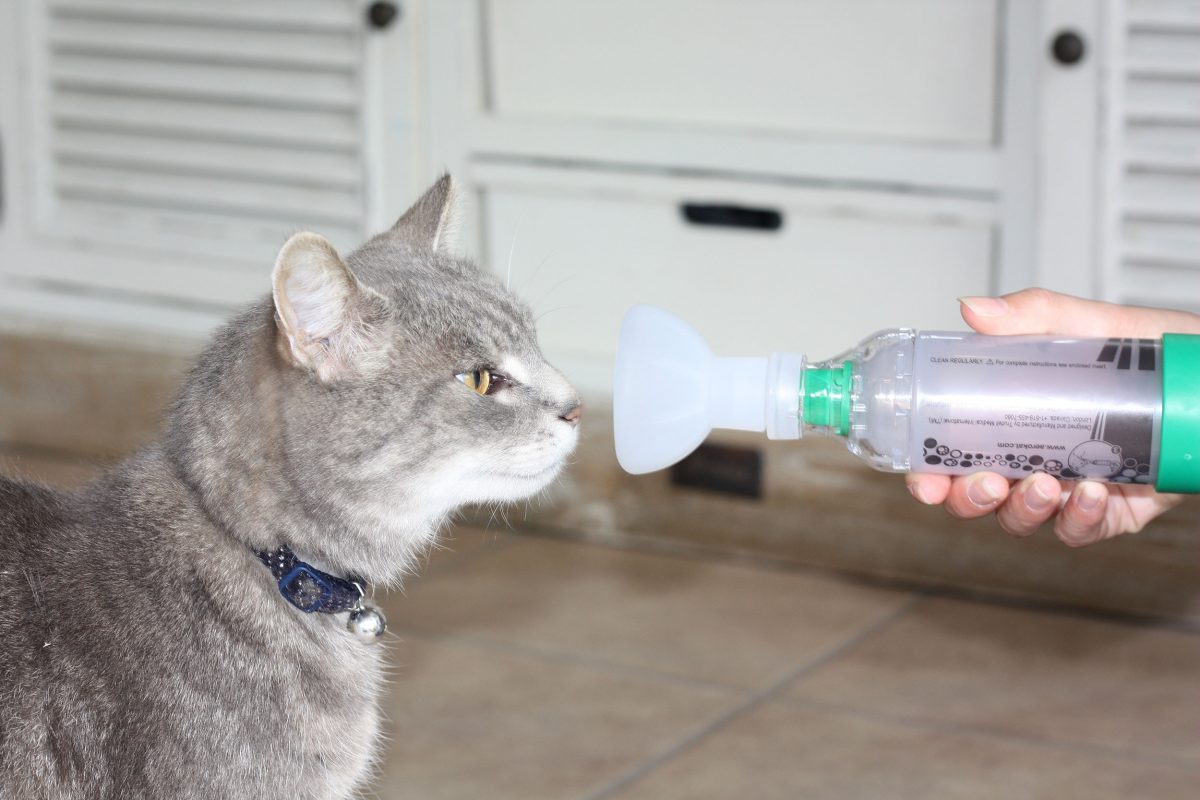
A special ‘spacer’ has been designed for the delivery of inhalational drugs to cats (see https://www.trudellanimalhealth.com/) One end of the Aerokat spacer is specially made to allow a human metered-dose inhaler (MDI) to fit and deliver a dose of medication into the chamber (spacer). At the other end a face mask is attached with a valve that allows the cat to breathe in the medication from the chamber. One to two puffs (according to your vet’s instructions) of the MDI are administered into the chamber and then the face mask is held gently over the cat’s face so it can breathe in the medication for typically 10-15 seconds. This is usually performed twice daily. Most cats tolerate the procedure very well and with a little practice, it is much easier than administering tablets. The other advantage of inhaled drugs is that less is absorbed into the body, potentially avoiding some of the side effects, and getting the drug to where it is needed.
Training your cat to tolerate the spacer device
Before you start to use the spacer to deliver inhaled drugs to your cat, it is a good idea to simply get them used to using the spacer and face mask first, without any drugs. This may be a slow process, but as these conditions are life-long, it is well worth taking time now to train your cat to tolerate the device and treatment.
What is the prognosis for feline asthma or chronic bronchitis?
Most cats can be successfully treated, but often life-long therapy is required. Some cats with severe disease can suffer repeated episodes of breathing difficultly, which in the worse cases can prove fatal. Prompt treatment is important to prevent permanent lung damage, which will be harder to treat. If you are worried about your cat, seek veterinary advice.
Thank you for visiting our website, we hope you have found our information useful.
All our advice is freely accessible to everyone, wherever you are in the world. However, as a charity, we need your support to enable us to keep delivering high quality and up to date information for everyone. Please consider making a contribution, big or small, to keep our content free, accurate and relevant.
Support International Cat Care from as little £3
Thank you.
Donate Now


