Hyperadrenocorticism is also known as Cushing’s disease or Cushing’s syndrome.
It is an uncommon disease in cats that develops when there is a persistent excessive production of the hormone cortisol from the adrenal glands (located close to the kidneys in the abdomen).
This is most often caused by an abnormality of the pituitary gland (located at the base of the brain) which controls production of the adrenal gland hormones, along with many others. In some cases it will be due to an abnormality of the adrenal glands themselves.
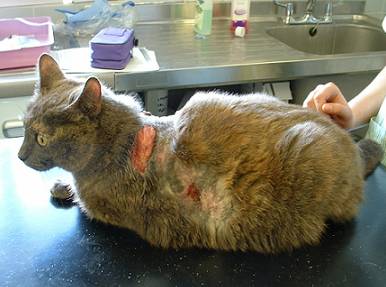
Cat showing wounds as a result of thin and fragile skin – a sign of Cushing’s disease
This disease is much more common in dogs than it is in cats, and is generally more difficult to control in cats than it is in dogs, although successful treatment is possible. The excessive cortisol concentrations can cause a variety of abnormalities including excessive thirst, weakness and skin changes.
Hyperadrenocorticism can also be induced by using high doses of cortisol-like hormones over a long period of time, as is sometimes necessary to control some diseases.
What causes hyperadrenocorticism?
Iatrogenic hyperadrenocorticism
Iatrogenic hyperadrenocorticism is the term used to refer to the disease when it is induced by the long-term administration of high doses of cortisol-like drugs. These drugs can be corticosteroids (often used to manage inflammation or allergies), but in cats progesterone-type drugs (progestagens) that are sometimes used to control reproductive cycling in entire female cats also have potent cortisol-like actions. If high doses of these drugs are used over a long period of time, they will have the same effect as occurs with naturally-occurring hyperadrenocorticism.
Naturally-occurring hyperadrenocorticism
Cortisol is a hormone produced in the body by the adrenal glands; two small glands situated just in front of the kidneys. Excess production of cortisol by the adrenal glands can be caused by an adrenal tumour or, more commonly, by a tumour affecting the pituitary gland (a small gland at the base of the brain). The pituitary gland produces a number of different hormones including adrenocorticotrophic hormone (ACTH), which stimulates the adrenal glands to produce cortisol. If a pituitary gland tumour results in excessive production of ACTH, this in turn will lead to the adrenals becoming enlarged and producing excessive cortisol.
When hyperadrenocorticism is caused by an adrenal tumour it is termed adrenal-dependent disease and when it is caused by a pituitary tumour it is termed pituitary-dependent disease. Adrenal-dependent disease accounts for less than 15% of naturally-occurring hyperadrenocorticism. When it is present, around half the cases will have an underlying malignant tumour (adrenal carcinoma). The majority of pituitary tumours causing the disease are benign and very tiny (microadenomas).
Clinical signs of hyperadrenocorticism
Naturally-occurring hyperadrenocorticism is uncommon in cats, and the iatrogenic form of the disease is also relatively uncommon as cats are quite tolerant of high doses of corticosteroids.
Naturally-occurring disease is seen primarily in middle-aged and older cats, and female cats are affected more commonly than males. Cortisol can have many different effects so clinical signs can be quite variable. Initial signs may be mild but they tend to progress over time. The most common signs are:
- Excessive drinking (polydipsia) and excessive urination (polyuria)
- Increased appetite
- Enlargement of the abdomen (a pot-bellied appearance)
- Lethargy
- Muscle wasting and weakness
- Poor coat condition
- Hair loss
- Curling of the ear tips
- Thin and fragile skin
In some affected cats, the skin can become so thin and fragile that it very easily bruises and can also very easily tear. Wounds may also be slow to heal.
Many cats with hyperadrenocorticism also have diabetes mellitus, because the excessive cortisol interferes with the effects of insulin. This may exacerbate the increased thirst and increased urination, and the hyperadrenocorticism may also make the diabetes more difficult to control. In fact, hyperadrenocorticism should always be considered in any diabetic cat that is proving difficult to manage.
Diagnosis of hyperadrenocorticism
Diagnosis of hyperadrenocorticism is not always straightforward and usually requires multiple blood tests, urine tests and diagnostic imaging (X-rays and/or ultrasound).
Routine blood tests may help to rule out more common causes of the clinical signs, after which more specific tests for hyperadrenocorticism may be done. These may include:
- Urine cortisol measurements – this can be used as a screening test to rule out hyperadrenocorticism, but high levels cannot confirm a diagnosis so further tests are needed.
- ACTH-stimulation test – with this test, blood samples are taken to measure cortisol levels before and after an injection of synthetic ACTH. If very excessive concentrations of cortisol are found then this usually confirms a diagnosis
- Dexamethasone screening test – with this test, blood cortisol levels are measured before and after an injection of dexamethasone (a potent corticosteroid that would normally suppress cortisol production). If cortisol production is not suppressed this may indicate hyperadrenocorticism is present.
- Measuring blood concentrations of ACTH – it may be possible to have blood concentrations of your cat’s ACTH measured which may also help to differentiate between adrenal- and pituitary-dependent disease
- X-rays and ultrasound – ultrasound especially can be useful as it is able to determine the size of the adrenal glands and evaluate whether one or both are enlarged. This can also help distinguish between adrenal- and pituitary-dependent disease
Unfortunately no single test is completely accurate and reliable in diagnosing hyperadrenocorticism, so more than one test is usually needed and sometimes tests have to be repeated.
Treatment of hyperadrenocorticism
If iatrogenic hyperadrenocorticism is present, it is usually managed by controlled gradual withdrawal of the corticosteroid or progestagen that is being administered. It may be necessary to find an alternative type of drug if it has been used to manage an allergy, for example.
With naturally-occurring hyperadrenocorticism a number of treatment options are available, but most commonly control of the disease will be attempted with drug therapy.
- Drug therapy with trilostane – a number of different drugs have been used to suppress cortisol production from the adrenal glands in cases of hyperadrenocorticism, but few of these work well in cats. Trilostane, which inhibits production of cortisol and is widely used in dogs, also appears to be effective in cats, and this is the most commonly used drug. Tablets have to be administered once or twice daily, and the dose adjusted according to response. Clinical signs may improve only gradually even with successful management of the disease
- Surgical adrenalectomy – this is the surgical removal of an adrenal gland, and this may be a good treatment option if just one adrenal gland is affected (for example if there is a benign tumour affecting one of the two adrenal glands)
- Hypophysectomy – this is the term used to refer to surgical removal of the pituitary gland – although technically possible, this is extremely difficult surgery that carries very high risks and is not generally recommended (and only available at a few specialist centres).
- Radiotherapy for pituitary tumours – where available, radiotherapy for an underlying pituitary tumour can help to control hyperadrenocorticism, although availability of this is limited.
What is the prognosis for cats with hyperadrenocorticism?
Hyperadrenocorticism is a serious disease and carries a guarded prognosis. The disease can rarely be cured, but with appropriate treatment a number of cats will respond well and may have many months or even years of excellent quality of life. If the underlying cause is a malignant adrenal tumour, inevitably the prognosis is more guarded.
Thank you for visiting our website, we hope you have found our information useful.
All our advice is freely accessible to everyone, wherever you are in the world. However, as a charity, we need your support to enable us to keep delivering high quality and up to date information for everyone. Please consider making a contribution, big or small, to keep our content free, accurate and relevant.
Support International Cat Care from as little £3
Thank you.
Donate Now


