What is hyperthyroidism?
Hyperthyroidism (overactive thyroid glands) is a very common disorder of older cats.
It is caused by an increase in production of thyroid hormones from the thyroid glands, which are situated in the neck.
Thyroid hormones are responsible for regulating many body processes and when too much hormone is produced the clinical signs can be quite dramatic, and cats can become seriously ill. Thyroid hormones also help control the body’s metabolic rate and cats with hyperthyroidism tend to burn up energy too rapidly and typically suffer weight loss despite having an increased appetite and increased food intake.
Fortunately, the vast majority of cats that develop hyperthyroidism can be treated very successfully and most cats will make a complete recovery.
What causes hyperthyroidism?
In the vast majority of cases hyperthyroidism in cats is caused by a benign (non-cancerous) change. Cats have two thyroid glands, and in most cases (more than 70%) both are involved in the disease, and become enlarged (a change called ‘nodular hyperplasia’, which resembles a very benign tumour). The underlying cause of this change is currently unknown, but is very similar to one of the two main causes of hyperthyroidism in humans called ‘toxic nodular goitre’.
Rarely (in less than 1-2% of cases) a malignant (cancerous) tumour (thyroid adenocarcinoma) can be the underlying cause of the disease.
Signs of hyperthryroidism
Hyperthyroidism is usually seen in middle-aged and older cats, rarely being seen in cats less than 7 years of age. Male and female cats are affected equally.
In affected cats, a wide variety of signs usually develop, but these are usually subtle at first, and become more severe over time as the underlying disease gets worse. Also, as it is mostly older cats that are affected, some cats will have other diseases that can complicate and even mask some of the clinical signs.
The ‘classic’ signs of hyperthyroidism are:
- Weight loss
- Usually a good or increased appetite (polyphagia)
- Increased thirst (polydipsia)
- Increased activity, restlessness or irritability
- An increased heart rate (tachycardia)
- A poor and unkempt hair coat
Mild to moderate diarrhoea and/or vomiting develop in some cats, and some will be noticeably intolerant of heat and seek out cooler places to sit. Some (especially advanced cases) may also pant when they are stressed, which is very unusual in cats.
Although most hyperthyroid cats show a good or increased appetite and restlessness, in some cases there may be generalised weakness, lethargy and loss of appetite.
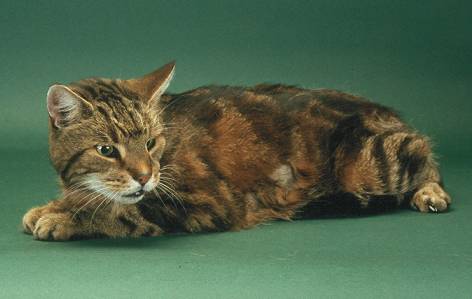
This cat is showing weight loss and poor coat – typical signs of hyperthyroidism
Complications of hyperthyroidism
Uncontrolled hyperthyroidism has important consequences on the heart, causing increased heart rate but also changes in the muscular wall of the heart that will eventually cause heart failure if untreated.
Hypertension (high blood pressure) is another potential complication of hyperthyroidism, although seen less commonly, and this can cause damage to several organs including the eyes, kidneys, heart and brain. If hypertension is diagnosed along with hyperthyroidism, drugs will be needed to control the blood pressure.
Kidney disease (chronic kidney disease) does not generally occur as a direct effect of hyperthyroidism, but the two diseases often occur together because they are both common in older cats. Care is needed where both these conditions are present, as managing hyperthyroidism can sometimes have adverse effects on kidney function.
Diagnosis
Although the thyroid glands usually enlarge with hyperthyroidism, this is not usually visible. Detection of enlarged glands will usually require careful palpation (examination by touch) by your vet. However, in some cats there is no obvious enlargement, often because the overactive tissue is in an unusual site (such as the chest cavity).
To confirm a diagnosis, a blood test is needed to measure the level of thyroid hormones in the blood. Usually, measuring the thyroxine (T4) concentration is all that is required to confirm a diagnosis, but sometimes additional tests may be needed (such as measurement of ‘free T4’ in the blood).
Other laboratory tests may also be abnormal – for example liver enzymes are commonly increased with hyperthyroidism, and both blood and urine tests are usually advised to help rule out concurrent problems (such as kidney disease). Blood pressure should also be checked where possible with hyperthyroid cats, and an electrocardiogram (ECG – electrical tracing of heart activity), and a chest X-ray or ultrasound may be helpful where heart disease is suspected.
Technetium scan
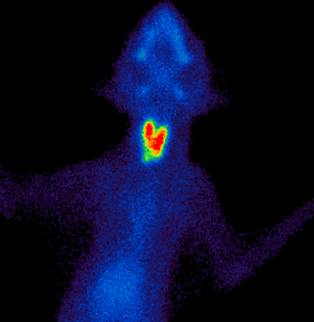
Technetium scan of a cat showing bilateral hyperthyroidism
A technetium scan is a technique that is available at some specialist centres, and can be useful in some hyperthyroid cats. This technique can help confirm a diagnosis, but importantly will locate exactly where the abnormal tissue is and so can be very helpful if surgery is being considered but where there is no clearly identifiable enlarged thyroid on examination.
A technetium scan involves injecting a very small dose of a radioactive chemical (technetium) into the cat’s vein. The technetium is selectively taken up by abnormal thyroid tissue, and this can be detected using a special camera (a ‘gamma camera’). This is a simple, safe and easy procedure.
Treatment
Successfully treated cats, irrespective of what treatment is used, will usually have complete reversal of all the signs of hyperthyroidism. Further evaluation will usually be needed to check kidney function and ensure long-term goals of thyroid hormone concentrations are being achieved, but most cats do remarkably well when treatment is administered. There are four main options for treatment, each with advantages and disadvantages:
Medical management (anti-thyroid drug therapy)
The most commonly used and effective anti-thyroid drugs belong to a group known as thioamides. This includes both methimazole and carbimazole that are widely used in the management of both feline and human hyperthyroidism. These drugs are available in tablet form and they reduce both the production and release of thyroid hormones from the thyroid gland. They do not provide a cure for, but they do allow either short-term or long-term control of hyperthyroidism. However, to maintain control of the disease medication has to be given at least on a daily basis (and often twice daily).
The treatment dose is adjusted to effect and these drugs are usually both safe and effective. Side effects are uncommon. Poor appetite, vomiting and lethargy are most commonly seen, and these effects often resolve after the first few weeks of treatment. However, if gastric irritation persists alternative treatment may be necessary. More serious problems (bone marrow suppression, liver disorders, or skin irritation) are rarely seen.
Even if other surgery or radioactive iodine is considered (see below), drug therapy is often used initially to monitor the effect of successful treatment on kidney function.
Surgical thyroidectomy
Surgical removal of the affected tissues (thyroidectomy) can produce a permanent cure and is a common treatment for many hyperthyroid cats. In general this is very successful and can produce a long-term or permanent cure in most cats. However, occasionally signs of hyperthyroidism develop again at a later time if previously unaffected thyroid tissue becomes diseased.
To reduce anaesthetic and surgical complications, where possible cats should initially stabilised with anti-thyroid drug therapy before surgery is performed. Any significant heart disease should also be managed. The major risk associated with the surgery itself is inadvertent damage to the parathyroid glands – these are small glands that lie close to, or within, the thyroid glands themselves, and have a crucial role in maintaining stable blood calcium levels. Because there is a small risk that temporary interference with calcium regulation may occur, it is usually recommended that cats remain hospitalised for a few days after surgery, and blood calcium concentrations are monitored during this time.
After surgery, occasional blood tests are recommended to ensure normal thyroid hormone levels are being maintained.
Radioactive iodine therapy
Radioactive iodine (I-131) is a very safe and effective treatment for hyperthyroidism. It has the advantage of being curative in most cases with no ongoing treatment. The radioactive iodine is administered as a single injection, usually simply given under the skin. The iodine is taken up by the active (abnormal) thyroid tissue, but not by any other tissues, resulting in a selective local accumulation of radioactive material in the abnormal tissues. The radiation destroys the affected abnormal thyroid tissue, but does not damage surrounding tissues or the parathyroid glands.
There are no significant side-effects with this treatment, but because cats are temporarily radioactive they have to be kept hospitalised for a short period after treatment as a precaution. Unfortunately, because this treatment requires handling of radioactive drugs it is also only available at certain centres.
A single injection of radioactive iodine is curative in around 95 per cent of all hyperthyroid cats, but following treatment occasional blood tests are recommended to ensure normal thyroid hormone levels are being maintained.
Dietary treatment
A new option that has more recently become available for managing hyperthyroid cats is to feed them on a special diet that has strictly controlled levels of iodine. As iodine is used by the thyroid gland to make thyroid hormones, if there is only sufficient iodine in the diet to make normal levels of these hormones, this can help to control the disease.
This is an interesting form of therapy that appears to be quite successful, at least in a number of cats. It does require feeding a special therapeutic diet that is only available from your vet, and cats need to consume this diet exclusively to ensure effective control. Nevertheless, many cats can have their disease controlled in this way and it is an alternative to other forms of therapy for a number of cats.
Treatment of thyroid adenocarcinoma
The rare cases of thyroid adenocarcinoma (malignant tumour of the thyroid) are more difficult to treat, but can sometimes be successfully managed using much higher doses of radioactive iodine.
Thank you for visiting our website, we hope you have found our information useful.
All our advice is freely accessible to everyone, wherever you are in the world. However, as a charity, we need your support to enable us to keep delivering high quality and up to date information for everyone. Please consider making a contribution, big or small, to keep our content free, accurate and relevant.
Support International Cat Care from as little £3
Thank you.
Donate Now



