The importance of good nutrition for aiding recovery in the hospitalised patient is undisputed, with ‘let food be thy medicine’ being a long-standing mantra in medical circles.
However, providing nutritional support to any critically ill patient presents challenges and, for the veterinary team caring for a feline patient with inappetence (ie, a reduced or absent appetite), there are some very specific requirements.
Inappetence is a common reason for a pet cat to be presented for veterinary attention; among ill, hospitalised cats, inappetence is even more frequently encountered. To ensure that nutrition is prioritised for any cat that is reluctant to eat, the International Society of Feline Medicine (ISFM) has today launched a suite of resources. These are centred on the 2022 ISFM Consensus Guidelines on Management of the Inappetent Hospitalised Cat, published in the Journal of Feline Medicine and Surgery.1 Complementing this state-of-the-art information are videos and guidance (available at bit.ly/inappetentcattoolkit) to assist the veterinary team, as well as cat owners and caregivers, to provide the best possible care.
It is imperative always to act quickly when a cat is showing loss of appetite, as even a few days of suboptimal nutrition can have severe consequences, potentially perpetuating illness, delaying recovery, slowing wound healing and compromising gut health and immunity. The authors of the new guidelines – an international panel of veterinary and behaviour experts – recognise that understanding ‘what makes a cat a cat’ is integral to obtaining a good outcome. While the most common causes of inappetence in cats are conditions leading to nausea, pain and/or ileus (reduced or absent gut motility), the stress of hospitalisation can itself lead to a reluctance to eat. This is not surprising when it is considered that pet cats retain many of the characteristics of their wildcat ancestors in being crepuscular (more active around dawn and dusk), territorial or ‘place bonded’, obligately carnivorous and selectively social. As such, they often do not cope well with change; this extends to their food preferences, which are set at an early age, commonly resulting in a dislike of unfamiliar tastes and textures. Moreover, the cat’s highly attuned senses, developed to create proficiency in hunting and survival, can easily become overwhelmed in the hospital clinic – an environment that, from the cat’s perspective, is intense, unfamiliar and signals danger, with no option to escape.

A cat eating in a hospital setting. Image: Samantha Taylor, BVetMed(Hons), CertSAM, DipECVIM-CA, MANZCVS, FRCVS
A common thread running through the new resources is that a ‘cat friendly’ ethos should always be at the centre of care, whether it is being provided in the clinic or at home. This is vital for ensuring mental wellbeing, which is inextricably linked to both physical health and appetite. Strategies for reducing stress in the veterinary clinic include noise reduction, gentle handling and provision of comfortable bedding, clean litter and somewhere to hide (for example, a box or a cat carrier placed in the cage, or simply a towel hung halfway across the cage door). During any interactions with the patient, the veterinary and nursing staff should move slowly, be predictable, calm and gentle, and talk softly. The guidelines stress the importance of creating positive associations by, for example, offering a treat, quiet words or stroking (assuming the cat responds positively to this) so that the patient learns that the cage is not only opened for a procedure.
A cat that is reluctant to eat should regularly be offered opportunities to eat, taking care to avoid overwhelming them with a ‘buffet’ selection of different foods, which can be aversive. Wiping food on the cat, in the hope they will lick it off, is never advisable, and syringe- or force-feeding is never appropriate.
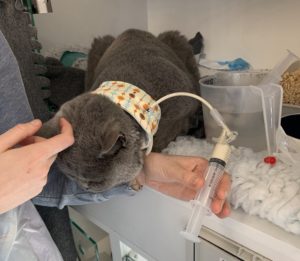
A hospitalised cat being fed via a feeding tube using a cat friendly approach. Image: Samantha Taylor, BVetMed(Hons), CertSAM, DipECVIM-CA, MANZCVS, FRCVS
In some cases, a feeding tube may be required to optimise recovery of an inappetent patient, and the guidelines and toolkit resources provide detailed practical advice on what, when and how to provide nutritional support in this way in order to safely promote calorie and nutrient intake, while minimising risks and complications. There is a particular focus on the placement and management of naso-oesophageal, nasogastric and oesophagostomy tubes, the last of which can be used by owners in the comfort and familiarity of the home setting. Irrespective of whether the cat is fed by tube at home or in the clinic, the principles are much the same: allow the patient to relax and settle as much as possible before feeding and provide reassurance by speaking quietly and calmly and, if the cat responds well to it, stroking or brushing. Also, never rush the feeding process, as this could cause negative associations with both feeding and handling.
Feline specialist Samantha Taylor, chair of the new guidelines, explains that the aim in developing these resources has been to provide veterinary professionals with confidence to place feeding tubes, and caregivers with vital information on caring for cats with inappetence. The message for her veterinary colleagues is to act promptly for any cat with a reduced appetite: ‘Don’t wait! Instead of hoping the cat will eat tomorrow, act today and improve patient outcomes.’
References
1. Taylor S, Chan DL, Villaverde C, et al. 2022 ISFM consensus guidelines on management of the inappetent hospitalised cat. J Feline Med Surg 2022; 24: 614–640. Available at: https://journals.sagepub.com/doi/full/10.1177/1098612X221106353






